Research
Epigenetic Studies
Device Development Studies
Correlation of Epigenetic Marks Between Human Brain Tissue and Peripheral Tissues

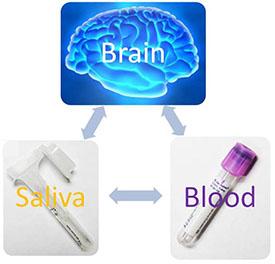
A challenge in psychiatric epigenetic studies is that the organ of interest is the brain, which, of course, is very difficult to access in live humans for the purpose of obtaining samples for DNAm analysis. Thus, we need to rely on peripheral tissues for our studies. However, it is not known whether DNAm changes in the periphery reflect what is happening in the brain. We, in collaboration with Iowa neurosurgeon Dr. Hiroto Kawasaki, are collecting brain tissues resected for the treatment of refractory epilepsy, together with saliva and blood taken before and after surgery, so that we can test DNAm correlation among them at specific loci. This could help determine which peripheral loci are most useful as markers for DNAm in brain.
Genome-wide DNA methylation comparison between live human brain and peripheral tissues within individuals- paper cited over 50 times since published in 2019.
Blog: Genome-wide DNA methylation comparison: Brain tissue vs. blood, saliva and buccal cells
Genome-Wide Epigenetic Investigation of High Dose Steroid Exposure in Humans
Genome-wide DNA methylation investigation of glucocorticoid exposure within buccal samples
Epigenetic Investigation of Stress in Depression and PTSD
It is highly likely that significant trauma leaves molecular marks in our system that lead to psychiatrically poor outcomes such as depression and PTSD. However, it is usually challenging to capture the influence of different kinds of trauma all together at the molecular level because, as opposed to using an animal model, it is hard to control potential confounders in human studies. Thus, it is crucial to identify a large cohort with a relatively uniform type of trauma. A research group from the Japanese National Defense Medical College has been studying their patient population over many years, with detailed clinical information including patients’ trauma history. In collaboration with this group, we are measuring DNAm to investigate the influence of trauma and its susceptibility to depression and PTSD.
Click here to watch Dr. Shinozaki’s video feature, describing our study.
Development of a point-of-care EEG device for early detection of delirium
Delirium is a prevalent and dangerous state of confusion that affects millions over 65 years of age. A lack of effective screening methods in high-volume hospital settings results in delirium being seriously underdiagnosed and undertreated. Undetected delirium in hospitalized elderly patients greatly increases mortality, length of stay, and rates of post-discharge institutionalization. One-year mortality rates after delirium can be as high as they are for heart attacks. Beyond those human health costs, annual financial losses due to delirium are estimated to be over $150 billion in the U.S. alone.
Current diagnostic and screening methods for delirium based on conventional 20-lead EEGs or various questionnaires have a number of drawbacks. The former is time-consuming, expensive, and cumbersome. The latter is also time-consuming, requiring many hospital staffs, thus expensive, and can be highly subjective. Thus, they are neither practical nor feasible for screening large volumes of hospitalized patients, even if limited only to high-risk populations. This project aims to prove the feasibility of developing an accurate/objective portable point-of-care (POC) device for delirium detection and screening in hospital settings. As envisioned, this new, bispectral EEG (“BSEEG”) system (using only a few EEG leads) would be rapid, objective, low-cost, and user-friendly. It would be based on a novel signal-processing algorithm that can detect delirium early on to save patients’ lives, hospital resources, and healthcare costs.
Our research team conducts a proof-of-concept project focused on developing a signal-processing algorithm/POC device for the mass screening of hospitalized elderly patients and for early detection of delirium. Their preliminary work has shown that BSEEG can provide good-quality brain wave signals that compare well to the signals obtained via conventional EEG in a matter of minutes vs. the hours or days it takes to administer and interpret standard EEGs. The team has also shown that preliminary analysis of the spectral density of brain waves from just two channels of a BSEEG can distinguish delirious patients from normal controls, as well as a delirious state from a recovered state for a single individual. Based on this strong preliminary data and the broad expertise of the R&D team, the Shinozaki Lab is, with the help from UI Research Foundation (UIRF), pursuing opportunity for commercialization of this technology so that this technology can be brought to the patients as soon as possible. In Sept 2015, UIRF has awarded GAP funding to the PI, Gen Shinozaki, to support this project.
Click here to read a Psychiatric News article featuring Dr. Shinozaki titled "Point-of-Care EEG Device Could Ease Efforts to Detect Delirium."
Mortality prediction by bispectral electroencephalography among 502 patients: its role in dementia
Topological data analysis (TDA) enhances bispectral EEG (BSEEG) algorithm for detection of delirium
Bispectral EEG (BSEEG) to assess arousal after electro-convulsive therapy (ECT)
Delirium detection by a novel bispectral electroencephalography device in general hospital
The point-of-care EEG for delirium detection in the emergency department
